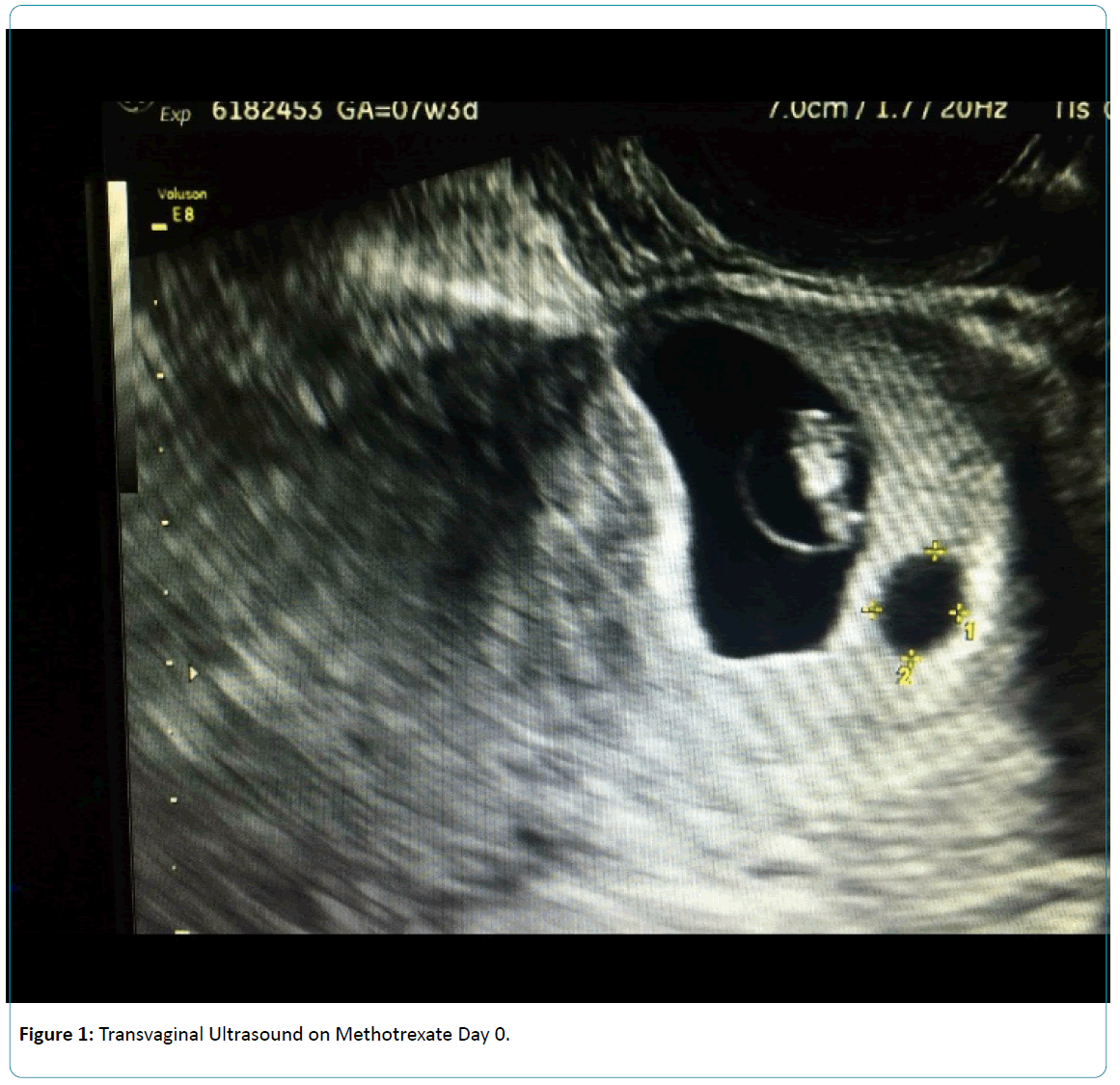
Successful Termination of a Cesarean Scar Ectopic Pregnancy with Systemic Methotrexate and Local Potassium Chloride Injection
Ann Schufreider and Eve C Feinberg
1Department of Obstetrics and Gynecology, The University of Chicago, 5841 S. Maryland Avenue, Chicago, IL, 60637, United States
2Fertility Centers of Illinois, 900 N. Kingsbury Ste RW6, Chicago, IL, 60610, United States
3Department of Obstetrics and Gynecology, NorthShore University Health System, 2650 Ridge Road, Evanston, IL, 60201, United States
- *Corresponding Author:
- Ann Schufreider
Department of Obstetrics and Gynecology
The University of Chicago 500, W. Superior
Unit 1609, Chicago, IL, USA
Tel: 847-204-1481
E-mail: Ann.Schufreider@uchospitals.edu
Received date: March 14, 2016; Accepted date: April 28, 2016; Published date: May 02, 2016
Citation: Schufreider A, et al. Successful Termination of a Cesarean Scar Ectopic Pregnancy with Systemic Methotrexate and Local Potassium Chloride Injection. J Reproductive Endocrinol& Infert. 2016, 1:8. doi: 10.4172/JREI.100008
Copyright: © 2016 Schufreider A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Cesarean Section Scar Ectopic Pregnancy (CSEP) is a rare but serious condition in which the embryo implants within the myometrium of a previous C-section scar. This can lead to maternal complications such as abnormal placentation, hemorrhage, or death due to uterine rupture. Despite these grave consequences, a standardized treatment protocol has not yet been established. The data remains limited given the rarity of the occurrence. This case report describes a patient who was diagnosed with a CSEP at 7 weeks gestation. She was successfully treated with a combination of systemic methotrexate, intra-gestational sac potassium chloride (KCl) instillation, and transvaginal aspiration of the gestational sac. This report adds to the growing body of literature on safe and effective treatments for CSEP.
Keywords
Ectopic pregnancy; Cesarean scar; Methotrexate; Potassium chloride
Introduction
Ectopic pregnancy accounts for 1%-2% of all pregnancies [1,2]. Those occurring within a previous Cesarean section scar are rare with potential fatal consequences and account for 0.05%-0.04% of all pregnancies [1]. While these types of ectopic pregnancies are rare, they are increasing as the Cesarean Section rates have risen in recent years [3]. The clinical presentation varies and up to 40% of cases are asymptomatic [4]. Early diagnosis and adequate treatment are crucial to maternal health and preservation of fertility. While it is recommended to terminate these pregnancies at the earliest possible time, no definitive therapeutic approach has been established [5]. Treatment options include medical therapies such as systemic methotrexate or surgical interventions such as scar wedge resection or hysterectomy [1,6]. This case report details a first trimester CSEP in which a combination of systemic methotrexate, intra-amniotic KCl injection, and gestational sac aspiration were employed to achieve a successful and safe outcome.
Case Report
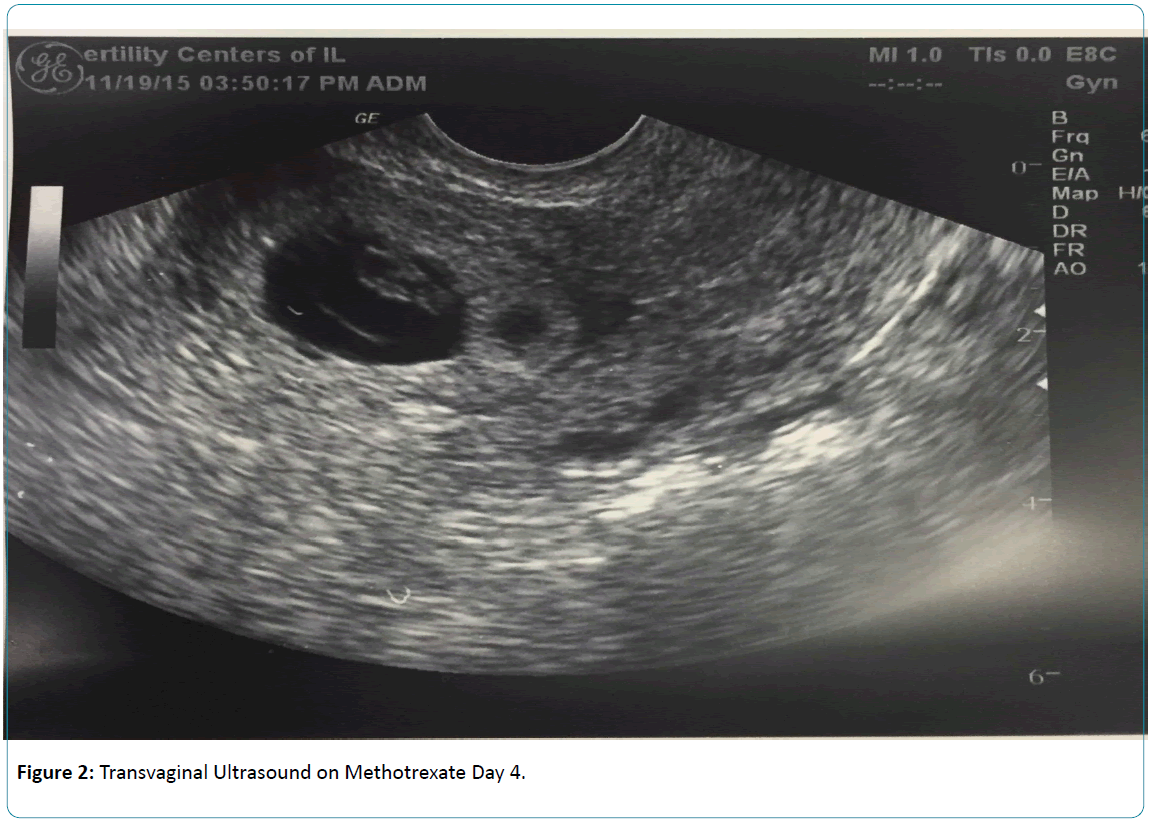
A 26 year old G41021 healthy female with a history of one prior term Cesarean Section for breech presentation was diagnosed with a CSEP during a routine first trimester ultrasound at 7 weeks 3 days gestation (Figure 1). She had reported some spotting in the previous weeks, but otherwise the pregnancy had been unremarkable. Her beta human chorionic gonadotropin (ß-hCG) level at the time of presentation was 58,641 mIU/mL. The patient was carefully counseled on both medical and surgical options. She refused to undergo surgery. After confirming a normal complete blood count (CBC) and liver/renal function tests, methotrexate 50 mg/m2 was administered as a single dose via intramuscular (IM) injection per the “2-dose” methotrexate protocol published by Barnhart et al. in 2007 [7]. On day 4 the patient’s ß-hCG level had increased to 63,907 mIU/mL and transvaginal ultrasound revealed the presence of fetal cardiac activity (FCA) (Figure 2). Given the rising ß-hCG and persistent FCA, a second dose of methotrexate was given and after careful counseling, the decision was made to proceed with instillation of KCl into the gestational sac. The patient was given IV sedation and using a transvaginal ultrasound probe equipped with a needle guide, a Cook 17 gauge double lumen ovum aspiration needle was introduced transvaginally and into the gestational sac. The needle was connected to KCl for instillation and to a Rocket aspiration pump for suction. Five milliliters of KCl was first injected into the amniotic sac to disrupt fetal cardiac activity and then the gestational sac was gently aspirated until collapse. Upon withdrawal of the needle, there was hemostasis and no immediate complications. Similar ultrasound guided procedures have been described in the literature [8]. The patient was sent home.
Four days after the procedure the patient presented to the Emergency Room complaining of 2 days of myalgias, sore throat and fevers. She was afebrile on admission with only mild abdominal pain. Transvaginal ultrasound demonstrated absence of a fetus. There was presence of some solid material in the anterior lower uterine segment consistent with products of conception in the region of prior implantation within with Csection scar. Despite not having a visible fetal pole or yolk sac visualized, the ß-hCG that day had risen to 72,974 mIU/mL. CBC and blood chemistries were within normal limits. Given that we expected a decrease in the ß-hCG levels following 2 doses of methotrexate , KCL instillation, and sac aspiration the decision was made to administer another 50 mg/m2 dose of IM methotrexate. Her febrile illness was thought to be due to a viral syndrome unrelated to the ectopic pregnancy treatment. Seven days later, ß-hCG levels decreased to 12,401 mIU/mL and were followed weekly for 5 weeks until <1 mIU/mL.
Discussion
As mentioned previously, several treatment options exist for the treatment of CSEP, including both medical and surgical options. The surgical options include uterine wedge resection via a laparoscopic or open approach as well as hysteroscopic resection of the mass. The patient presented in this report desired to avoid surgical management and preferred a less invasive approach, therefore these options were not considered. Medical treatments are also available and include systemic methotrexate, local injection of methotrexate or embryocides, sac aspiration, or a combination of these methods [1].
The use of systemic methotrexate alone is the recommended medical therapy for select cases of tubal and cervical ectopic pregnancies; however its reported success rate with CSEP ranges from 57%-100% [5]. Several hypotheses for this variation in success have been proposed. First, the dense, fibrotic tissue of the gestational scar surrounding the ectopic pregnancy may inhibit penetration by methotrexate [5]. Second, there is heterogeneity in the protocols used to treat CSEP. Lam et al. reviewed case reports of CSEP in which methotrexate therapy alone was used in order to indentify common factors in treatment failure. They reported a 25% failure rate from the 12 cases included and no commonalities were identified [9].
Given the rarity of cases, no consensus exists on risks factors for methotrexate failure in CSEP cases. However, several risk factors for methotrexate failure have been indentified in tubal ectopic pregnancies, and this information may be extrapolated to CSEP cases. These risk factors include the presence of an embryo, day 1 ß-hCG level of ≥3,000 mIU/mL, presence of fetal cardiac activity, gestational mass >4 cm, and continued rapid rise in ß-hCG level during methotrexate therapy [10,11]. These risk factors explain why we chose a multi-faceted approach to treatment. Given that our patient had an elevated ß-hCG level as well as fetal cardiac activity, methotrexate therapy alone was unlikely to be successful.
Alternative therapies such as gestational sac aspiration or instillation of local agents have been explored to avoid surgical intervention. In 2009 Taskin et al. published a review article concerning treatment of heterotopic CSEP [12]. They included 5 cases between 6-10 weeks gestational age that were all treated with local KCl injection. All were delivered by Cesarean Section of which three were complicated by massive hemorrhage. One additional case was treated with embryo aspiration at five to six weeks gestation. The result was a hysterectomy at the time of Cesarean Section due to hemorrhage from the lower uterine segment. While many of these cases resulted in a viable fetus, they were also accompanied by massive maternal hemorrhage. Such a case was described by Wang et al. in which a heterotopic CSEP treated with local KCl resulted in a viable preterm infant, but the mother underwent a bilateral internal iliac artery ligation after losing more than 4 L of blood at the time of CS [13]. Therefore using only local therapy with KCl or sac aspiration can lead to significant maternal risks most commonly in the form of hemorrhage.
Given the unreliable success and accompanying risks of systemic methotrexate or KCl alone, using both to assist in terminating a CSEP has been utilized such as in our case. In 2015 Pirjani et al. presented four cases ranging in gestational age from 7 to 11 weeks [6]. All patients were all treated with local KCl (2.5 cc 50%) followed by systemic methotrexate. Two of the cases employed intracardiac KCl injections while the others injected into the amniotic sac. The time to reach nondetectable ß-hCG levels ranged from eight to eleven weeks. Interestingly there was no consensus among the cases regarding the dose or administration timeline of methotrexate. While most clinicians are familiar with the single dose, two dose, and multidose methotrexate regimens, those have been studied mostly in tubal ectopic pregnancies [11]. Therefore, the methotrexate dosage and timing may need to be adjusted in CSEP patients. For example, in our patient we employed the “2-dose methotrexate method” [7]. However, four days after the patient’s second methotrexate dose, her ß-hCG level was still rising. Since the patient had refused surgery and was hemodynamically stable, our best option was to administer another methotrexate dose.
We believe our treatment protocol would be applicable to future patients who fit the following criteria. They must be hemodynamically stable, have no contraindications to methotrexate, be reliable for follow up, and desire to avoid surgery. A third or fourth dose of methotrexate could be given in accordance to the “2 dose” methotrexate protocol published by Barnhart et al. [7]. Once ß-hCG levels have decreased by >15% from the prior measurement then we would recommend obtaining weekly ß-hCG levels until it reaches <1 mIU/mL. If at any point during treatment or follow up the patient experienced hemodynamic instability or severe abdominal pain we would recommend urgent surgical management. Additionally, if after 4 doses of systemic methotrexate the ß-hCG level were still rising, fetal cardiac activity were still present, or the gestational mass were increasing in size we would consider surgical intervention.
Our case represents an important contribution to the growing body of literature on CSEP treatment. Our use of systemic methotrexate, local KCl injection, and sac aspiration is an example of a safe and effective therapy to terminate a first trimester CSEP that maintains a woman’s fertility.
References
- Rotas M, Haberman S, Levgur M (2006) Cesarean Scar Ectopic Pregnancies:Etiology, Diagnosis, and Management. ObstetGynecol107:1373-1381.
- Santos-Ribeiro S, Tournaye H, Polyzos NP (2016)Trends in ectopic pregnancy rates following assisted reproductive technologies in the UK: a 12-year nationwide analysis including 160 000 pregnancies. Hum Reprod 31:393-402.
- World Health Organization and Human Reproduction Programme (2015) WHO statement on caesarean section rates: Executive summary.
- Rheinboldt M, Osborn D, Delproposto Z (2015)Cesarean Section Scar Ectopic Pregnancy: A Clinical Case Series. J Ultrasound 18:191–195.
- Riaz R, Williams TR, Craig BM, Myers DT (2015)Cesarean Scar Ectopic Pregnancy: Imaging, Features, Current Treatment Options, and Clinical Outcomes. Abdom Imaging 40:2589–2599.
- Pirjani R, Bayani L, Shirazi M (2015) Successful Local and Systemic Medical Treatment of Cesarean Scar Pregnancy and a Subsequent Term Pregnancy after Treatment: A Case Series. Iran J Reprod Med 13:445-450.
- Barnhart K, Hummel AC, Sammel MD, Menon S, Jain J, et al. (2007) Use of "2-dose" regimen of methotrexate to treat ectopic pregnancy. FertilSteril 87:250-256.
- Doubilet PM, Benson CB, Frates MC, Ginsburg E (2004)Sonographically Guided Minimally Invasive Treatment of Unusual Ectopic Pregnancies. J Ultrasound Med23:359–370.
- Lam P, Lo K, Lau T (2004) Unsuccessful Medical Treatment of Cesarean Scar Ectopic Pregnancy with Systemic Methotrexate: A Report of Two Cases. ActaObstetGynecolScand 83:108–111.
- Dilbaz S, Caliskan E, Dilbaz B, Degirmenci O, Haberal A (2006) Predictors of methotrexate treatment failure in ectopic pregnancy. J Reprod Med51:87-93.
- The Practice Committee of the American Society for Reproductive Medicine (2013) Medical treatment of ectopic pregnancy: a committee opinion. FertilSteril 100:638-644.
- Taskin S, Taskin EA, MD, Ciftci TT (2009) Heterotopic Cesarean Scar PregnancyHow Should It Be Managed? ObstetGynecol Sur 64:690-695.
- Wang CN, Chen CK, Wang HS, Chiueh HY, Soong YK (2007)Successful Management of Heterotopic Cesarean Scar Pregnancy Combined with Intrauterine Pregnancy after In Vitro Fertilization–Embryo Transfer. FertilSteril 88:e13-6.
- Goynumer G, Gokcen C, Senturk B, Turkgeldi E (2009) Treatment of a Viable Caesarean Scar Pregnancy with TransvaginalMethotrexate and Potassium Chloride Injection. Arch GynecolObstet280:869–872.
Open Access Journals
- Aquaculture & Veterinary Science
- Chemistry & Chemical Sciences
- Clinical Sciences
- Engineering
- General Science
- Genetics & Molecular Biology
- Health Care & Nursing
- Immunology & Microbiology
- Materials Science
- Mathematics & Physics
- Medical Sciences
- Neurology & Psychiatry
- Oncology & Cancer Science
- Pharmaceutical Sciences